7 Silent Signs of Gum Disease Most People Ignore
In my years of practice as a periodontist, I have sat across from countless patients who share a similar story. They come into my office, slightly anxious, and say, “Dr. Moshrefi, I didn’t think it was a big deal until my tooth started moving,” or “I thought bleeding when I flossed was normal.” It is a conversation I have had more times than I can count, and it highlights a fundamental misunderstanding about oral health that pervades our society.
Periodontal disease, commonly known as gum disease, is often referred to as a “silent killer” of teeth. Unlike a cavity, which might send a sharp jolt of pain through your jaw when you sip cold water, gum disease can progress for years without causing any significant discomfort. By the time pain actually sets in, the damage is often advanced. This is why understanding early gum disease symptoms is absolutely critical for preserving not just your smile, but your overall systemic health.
I am writing this because I believe in empowering my patients with knowledge. If you are reading this, you might be worried about a specific symptom, or perhaps you are just proactive about your health. Regardless of your motivation, identifying these silent signs early is the most effective way to avoid invasive treatments later. Let’s explore the indicators that your body is fighting a battle against bacteria—signs that act as the “check engine” light for your mouth.
The Physiology of Silence: Why You Don’t Feel Pain
Before we discuss the specific signs, it is important to understand why gum disease is so deceptive. I often been asked how a disease can destroy bone and gum tissue without hurting. The answer lies in the nature of the infection. Periodontal disease is a chronic inflammatory response to bacterial biofilm (plaque) and calculus (tartar). In the early stages, known as gingivitis, the nerves inside the teeth remain protected. The inflammation occurs in the soft tissues surrounding the teeth.
It is only when the infection advances to periodontitis—attacking the periodontal ligament and the alveolar bone—that the structural integrity of the tooth is compromised. Even then, the disease can be surprisingly painless until an acute abscess forms. This silent progression is why regular screenings are vital, and why you must be hyper-aware of the subtle changes I am about to outline.
1. “Pink in the Sink”: Bleeding During Brushing or Flossing
The most common sign I see, and the one most easily rationalized by patients, is bleeding gums. Many people believe that if their gums bleed when they floss, it is because they are flossing “too hard” or because they have not flossed in a while. While there is a grain of truth to mechanical trauma causing bleeding, healthy gums should not bleed under normal brushing and flossing conditions.
When bacterial plaque accumulates along the gumline, your immune system deploys white blood cells to fight the bacteria. This causes the gum tissue to become engorged with blood, ulcerated, and fragile. When you run a piece of floss against this inflamed tissue, the ulcerated lining breaks, causing bleeding. If you notice “pink in the sink” after spitting out your toothpaste, consider this a red flag. It is often the very first of the early gum disease symptoms appearing before any permanent damage is done.
2. The “Long Tooth” Look: Gum Recession
Have you ever looked in the mirror and thought that a specific tooth looks longer than it used to? Or perhaps you have noticed “black triangles” appearing between your teeth near the gumline. This is gum recession, and it is a hallmark of periodontal progression.
Gum tissue does not just pull back on its own; it pulls back because the underlying bone is shrinking away from infection, or because mechanical trauma and inflammation are destroying the attachment fibers. As the gum recedes, the root of the tooth becomes exposed. Unlike the crown of your tooth, which is covered in durable enamel, the root is covered in cementum, which is much softer and more vulnerable to decay. While recession can occur slowly over decades, rapid recession is a sign of active periodontal breakdown that requires immediate intervention.
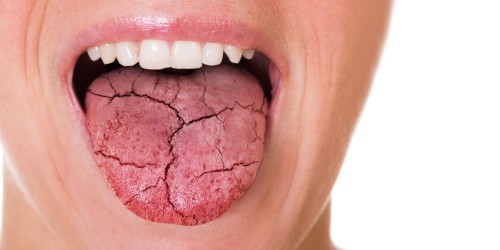
3. Persistent Halitosis: Bad Breath That Won’t Go Away
We all wake up with “morning breath,” but I am talking about a persistent odor that does not disappear after brushing, flossing, or using mouthwash. I often see patients who are incredibly self-conscious about this, chewing gum constantly to mask the issue. However, bad breath (halitosis) in the context of gum disease is caused by specific types of bacteria.
These pathogenic bacteria reside deep within the pockets between your teeth and gums—areas your toothbrush simply cannot reach. As these bacteria break down food particles and tissue, they release Volatile Sulfur Compounds (VSCs). These compounds smell like rotten eggs. If you have chronic bad breath, it is likely not because of what you ate for lunch, but because of a bacterial colony thriving beneath your gumline.
4. Heightened Sensitivity to Temperature
Sensitivity is a symptom that brings many people into my office. When you drink hot coffee or eat ice cream, do you feel a sharp, lingering zinger? While this can be caused by cavities or cracked teeth, it is frequently associated with periodontal issues. As I mentioned earlier regarding recession, when the gums pull back, the root surfaces are exposed.
The roots of your teeth contain thousands of microscopic tubules that lead directly to the nerve center of the tooth (the pulp). When the protective gum tissue is lost due to disease, external stimuli like heat, cold, or even sweets can travel through these tubules and irritate the nerve. Treating the sensitivity with special toothpaste is only masking the symptom; we need to address the reason the root was exposed in the first place.
5. Changes in Your Bite or Shifting Teeth
This is a symptom that usually indicates the disease has progressed from gingivitis to periodontitis. Patients often tell me, “My teeth feel different when I close my mouth,” or “I have a gap here that wasn’t there last year.”
Your teeth are held in place by the jawbone and the periodontal ligament. When gum disease destroys this supporting bone, the teeth lose their stable foundation. They may begin to drift, rotate, or flare outward. If you have noticed that your bite feels “off” or that food is getting stuck in gaps that didn’t exist previously, this is a sign of significant bone loss. At this stage, we are not just fighting inflammation; we are fighting to save the teeth from extraction.
6. Red, Swollen, or Tender Gums
Healthy gums should be firm, pink (though the shade varies by complexion), and stippled like the surface of an orange. They should fit snugly around the tooth like a turtleneck sweater. If your gums appear puffy, shiny, bright red, or dusky purple, they are inflamed.
This swelling is the body’s inflammatory response to the bacteria. While it might feel tender to the touch, it is often not acutely painful, leading many to ignore it. However, this chronic inflammation is dangerous. The Centers for Disease Control and Prevention (CDC) notes that 47.2% of adults aged 30 years and older have some form of periodontal disease. This swelling is the visible tip of the iceberg, signaling that the immune system is overwhelmed.
7. Deep Periodontal Pockets
This is a sign you cannot see in the mirror, but it is the most clinical definitive sign we look for. During an examination, I use a small ruler called a periodontal probe to measure the space between your tooth and gum. In a healthy mouth, this sulcus depth is between 1 to 3 millimeters.
When bacteria accumulate, they detach the gum from the tooth, creating a “pocket.” If these pockets measure 4 millimeters or more, you have gum disease. Bacteria in a 5mm or 6mm pocket cannot be removed by brushing or flossing. They form a hardened ecosystem that eats away at the bone. If you have been told you have “deep pockets” during a hygiene cleaning, do not take it lightly. It means the physical barrier of your oral health has been breached.
The Progression of Disease: A Clinical Overview
To help you visualize what is happening beneath the surface, I have compiled this breakdown of how the disease advances from reversible symptoms to permanent damage. Understanding where you might fall on this spectrum is the first step toward recovery.
| Stage | Clinical Description | Typical Symptoms | Reversibility |
|---|---|---|---|
| Gingivitis | Inflammation of the soft tissue only. No bone loss. | Bleeding, redness, puffy gums. | Fully Reversible with professional cleaning and home care. |
| Early Periodontitis | Infection spreads to bone. Pocket depths 3-5mm. | Recession, persistent bad breath, slight bone loss. | Manageable; damage can be halted but bone does not regrow naturally. |
| Moderate Periodontitis | More significant destruction. Pocket depths 5-7mm. | Teeth may feel loose, visible gaps, pus discharge. | Requires deep cleaning (scaling & root planing) and potentially surgery. |
| Advanced Periodontitis | Severe bone loss (50%+). Pocket depths 7mm+. | Shifting teeth, pain on chewing, risk of tooth loss. | Urgent surgical intervention or extraction required. |
Why Identifying Early Gum Disease Symptoms Can Save Your Life
I want to pause here and emphasize that this is not just about your teeth. As a medical professional, I look at the mouth as the gateway to the entire body. The inflammation occurring in your gums does not stay in your gums. The inflammatory markers and bacteria enter your bloodstream and travel to distant organs.
Scientific research has firmly established links between periodontal disease and major systemic health issues. For example, individuals with gum disease have a significantly higher risk of cardiovascular disease. The inflammation in the mouth contributes to the buildup of arterial plaque. Furthermore, for patients with diabetes, it is a two-way street: diabetes makes gum disease worse, and severe gum disease makes it harder to control blood sugar levels.
Another critical fact to consider is the specific bacteria involved. Porphyromonas gingivalis, a primary pathogen in chronic periodontitis, has been found in the brains of Alzheimer’s patients, suggesting a potential link between oral health and cognitive decline. By spotting early gum disease symptoms and treating them, you are effectively lowering your total body inflammatory burden.
Why “Wait and See” is a Dangerous Strategy
In dentistry, procrastination is the most expensive habit you can have. I often see patients who noticed bleeding gums two years ago but waited until a tooth became loose to schedule an appointment. At the early stage (Gingivitis), the treatment is often as simple as a rigorous professional cleaning and improved home hygiene. The cost is low, and the recovery is immediate.
Once the disease progresses to Periodontitis, we are no longer talking about simple prevention. We are looking at Scaling and Root Planing (deep cleaning), antibiotic therapy, or regenerative surgery to rebuild lost bone. The biological cost is the loss of your natural support structures, which can never be fully replicated by technology.
How We Treat Gum Disease at MD Perio
If you have recognized any of the signs I listed above, please do not panic. Anxiety often leads to avoidance, and I want you to feel empowered to take action. At MD Perio, we utilize the most advanced technologies to treat gum disease aggressively but gently.
We start with a comprehensive periodontal evaluation. This isn’t just a quick look; we measure every pocket, assess your bone levels with digital imaging, and review your systemic health history. For many patients, we can utilize non-surgical therapies, such as laser-assisted periodontal therapy, which eliminates bacteria and stimulates healing with minimal discomfort.
For more advanced cases, I specialize in regenerative procedures. We can use guided tissue regeneration and bone grafting to restore what the disease has taken away. My goal is always to save your natural teeth whenever possible and to restore your mouth to a state of health where you can smile, eat, and live without worry.
Next Steps: Reclaiming Your Oral Health
Ignoring the dashboard warning lights in your car eventually leads to an engine breakdown. Ignoring the silent signs of your body leads to health crises that are far more difficult to solve. If you have noticed bleeding, recession, bad breath, or any shifting in your teeth, your body is telling you it needs help.
You do not have to live with the fear of losing your teeth. Periodontal disease is treatable, and with the right care, it is controllable. By addressing these early gum disease symptoms now, you are investing in your longevity and your quality of life.
For more information on periodontal health and systemic links, I recommend reading resources from the American Academy of Periodontology, which provides excellent patient guides.
About Dr. Abdy Moshrefi
Dr. Abdy Moshrefi is a leading Periodontist and the founder of MD Perio in Los Angeles. With a focus on microsurgical techniques and implant dentistry, Dr. Moshrefi is dedicated to providing the highest level of periodontal care. He is known for his compassionate approach and his commitment to using state-of-the-art technology to ensure optimal patient outcomes. His practice focuses on saving teeth, regenerating lost bone and gum tissue, and restoring smiles with dental implants when necessary.
Ready to Stop Gum Disease in Its Tracks?
If you are in the Los Angeles or Beverly Hills area and are concerned about the signs discussed in this article, I invite you to visit us at MD Perio. Do not let fear keep you from the health you deserve.
Disclaimer: The content provided in this blog post is for informational purposes only and does not constitute medical or dental advice. It is not intended to replace professional diagnosis or treatment. Always seek the advice of your dentist, periodontist, or other qualified health provider with any questions you may have regarding a medical condition.
- The Real Cost of Dental Implants in Beverly Hills - March 2, 2026
- 7 Silent Signs of Gum Disease Most People Ignore - March 2, 2026
- Gum Recession Treatment Options: Which Is Right for You? - February 28, 2026
 (310) 859-9449
(310) 859-9449 7 Silent Signs of Gum Disease Most People Ignore
7 Silent Signs of Gum Disease Most People Ignore