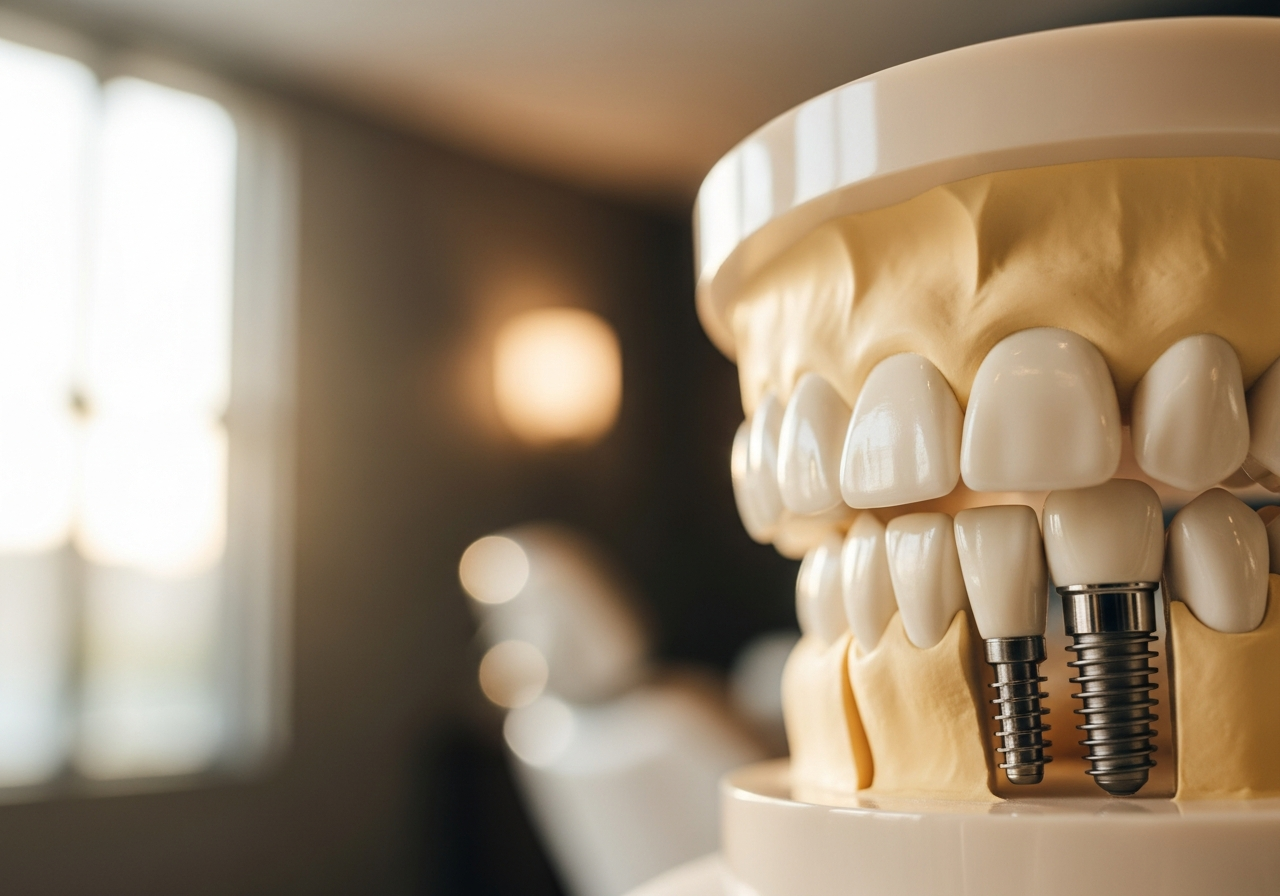
As a periodontist, I spend a lot of time talking to patients about how to restore their smiles. Without a doubt, dental implants are the gold standard for replacing missing teeth. They look natural, feel strong, and allow you to eat the foods you love. In fact, one of the most encouraging things I tell my patients is that dental implants have an incredibly high success rate—typically between 95% and 98%.
However, like any medical procedure, biology is unique to every person. While rare, complications can happen. When a patient comes to me worried about their implant, the first thing I want to do is put their mind at ease. Understanding the “why” is the first step toward fixing the issue. By exploring the common dental implant failure causes, we can work together to prevent them and ensure your smile lasts a lifetime.
In this guide, I am going to walk you through the five most common reasons implants might face challenges and, more importantly, how we can prevent these issues before they start.
1. Peri-Implantitis: The Impact of Gum Disease
You may have heard of gum disease (periodontitis) regarding natural teeth, but did you know it can affect implants too? We call this condition Peri-implantitis. In my practice, this is one of the leading factors I look for when an implant isn’t healing correctly.
Peri-implantitis is an inflammatory process that affects the soft tissue and the bone surrounding the dental implant. It is usually caused by the same bacteria that cause regular gum disease. If plaque and tartar build-up around the implant site, the bacteria can trigger an infection. This infection causes the gums to pull away from the implant and can eventually eat away at the bone holding the implant in place.
How We Prevent It
The good news is that peri-implantitis is largely preventable. I always emphasize that just because an implant is artificial doesn’t mean you can stop brushing and flossing. In fact, you need to be even more diligent.
- Daily Hygiene: Brushing twice a day and flossing around the implant is non-negotiable. I often recommend a water flosser to my patients as it helps clean those hard-to-reach areas around the crown.
- Regular Cleanings: You need to see your dentist and hygienist regularly. We have special tools to clean implants without scratching the surface, which prevents bacteria from finding a place to hide.
- Early Detection: If you notice bleeding, redness, or swelling around your implant, call me immediately. Catching this early is key to reversing the inflammation.
2. Failure to Osseointegrate: The Healing Process
This sounds like a complicated medical term, but osseointegration is actually a beautiful natural process. It comes from the Greek words osteon (bone) and integrare (to make whole). It refers to the structural and functional connection between the living bone and the surface of the load-bearing artificial implant.
When I place a titanium implant, your body is supposed to grow bone cells right up against the metal surface, locking it in place. This usually happens over a period of 3 to 6 months. However, sometimes the bone fails to fuse with the implant. This is often one of the primary dental implant failure causes shortly after surgery.
Why Does This Happen?
Several factors can interrupt this healing process. One of the most significant antagonists to osseointegration is smoking. Nicotine constricts blood vessels, which reduces blood flow to the gums and bone. Oxygen and nutrients are vital for healing, and smoking cuts off that supply.
Data Point: Research indicates that smokers have a significantly higher risk of implant failure compared to non-smokers. Studies suggest that the failure rate in smokers can be up to 20% higher than in non-smokers due to poor healing and increased risk of infection.
Ensuring Strong Bone Fusion
To prevent this, I conduct a thorough evaluation of your bone density before we even schedule the surgery. If your bone is too thin or soft, we might need to perform a bone graft first to build a solid foundation. Additionally, I strongly advise my patients to stop smoking—or at least pause significantly—during the healing period to give the implant the best chance of success.
3. Underlying Medical Conditions and Medications
Your oral health is a window to your overall health. When I review your medical history, I am not just being nosy; I am looking for systemic conditions that could act as dental implant failure causes. Certain autoimmune diseases and chronic conditions can affect how your body heals.
Uncontrolled Diabetes: This is a major factor. Patients with uncontrolled diabetes have a slower healing response and are more prone to infections. High blood sugar levels can impair the white blood cells needed to fight off bacteria at the implant site.
Osteoporosis and Medications: While osteoporosis (weakening of bones) itself isn’t always a deal-breaker, the medications used to treat it can be. Bisphosphonates, a common class of drugs for bone density, can sometimes lead to a rare condition called osteonecrosis of the jaw, which prevents healing.
Collaborative Care is Key
I believe in a holistic approach. If you have diabetes, it doesn’t mean you can’t have implants. It just means we need to work with your primary care physician to ensure your blood sugar levels are well-controlled (typically checking your HbA1c levels) before surgery. By managing your systemic health, we create a safe environment for your dental implant to thrive.
For more detailed information on how systemic diseases affect oral health, you can read this comprehensive overview from the National Institutes of Health (NIH) regarding risk factors in implant dentistry.
4. Occlusal Overload: The Pressure of Grinding
Imagine building a fence post. If you start shaking the post violently before the concrete at the base has dried, the post will never become stable. The same logic applies to your mouth. This is what we call “Occlusal Overload.”
Many of my patients suffer from Bruxism—the medical term for clenching or grinding teeth, often during sleep. Because you are asleep, you might not even know you are doing it. However, the force exerted during grinding is immense. Natural teeth have a ligament that acts as a shock absorber, allowing them to move slightly under pressure. Dental implants, however, are fused directly to the bone. They have no shock absorber.
If excessive force is applied to the implant, especially during the healing phase or even years later, it can cause the bone around the implant to fracture or recede. This can lead to the implant becoming loose.
Protecting Your Investment
Identifying this problem is a big part of my planning process. If I see signs of wear on your natural teeth, I will suspect grinding. To prevent failure from occlusal overload, I carefully adjust the bite of the new implant crown so it doesn’t take the brunt of your chewing force. Furthermore, I almost always prescribe a custom-made night guard for my patients with implants. Wearing this simple appliance at night acts as a cushion, protecting both your natural teeth and your implants from excessive force.
5. Lack of Sufficient Bone Volume
For a screw to hold tight in a wall, the wall needs to be thick enough to grip it. Similarly, an implant needs a specific volume of bone to encompass it completely. If there is not enough height, width, or density of the jawbone, the implant cannot stabilize.
Bone loss can occur for many reasons. If you had a tooth extracted years ago and never replaced it, the jawbone in that area naturally shrinks over time because it is no longer being stimulated by the tooth root. This atrophy is very common.
The Solution: Building a Foundation
Years ago, low bone volume meant you couldn’t get implants. Today, that is rarely the case. Using advanced 3D imaging (CBCT scans), I can see the exact dimensions of your bone before we start. If I see a deficiency, we use bone grafting techniques.
Bone grafting involves placing bone material—either from another part of your body, a donor, or synthetic material—into the area where the implant will go. Over a few months, your body absorbs this material and replaces it with your own new, healthy bone. This ensures that when we do place the implant, it is anchored in solid rock, not sand.
Recognizing the Signs of Trouble
I want you to feel empowered to monitor your own oral health. While regular check-ups with me are vital, you are the one living with your smile every day. Recognizing the early warning signs of potential failure can make the difference between saving an implant and losing it.
Here is what you should look out for:
- Pain or Discomfort: Some discomfort is normal right after surgery, but pain that persists or starts months later is a red flag.
- Mobility: If the implant feels loose, even slightly, when you touch it with your tongue or finger, contact me immediately. A healthy implant should be immobile.
- Swelling or Inflammation: Puffy, red gums around the metal post indicate infection.
- Difficulty Chewing: If it hurts to bite down, the implant may not be handling the pressure correctly.
Can a Failed Implant Be Replaced?
I often see the panic in a patient’s eyes when they think an implant has failed. They worry they are doomed to wear a denture forever. I am here to tell you that is usually not the case. If an implant fails, we can often remove it, clean the area, and allow the bone to heal.
Once the site is healthy again—which might involve a round of antibiotics or a bone graft—we can frequently attempt a second placement. Success rates for second attempts are generally good, provided we have identified and addressed the original cause of the failure, such as improved hygiene or better diabetes management.
Partnering for Your Long-Term Success
I view dental implants as a partnership between doctor and patient. My job is to perform the surgery with precision, use the highest quality materials, and ensure the biology is right. Your job is to maintain that environment through excellent home care and lifestyle choices.
It is important to remember that while we have discussed dental implant failure causes, the vast majority of my patients enjoy their implants for decades without a single issue. Technology in our field is better than ever, and our understanding of how to prevent these problems grows every year.
If you are considering implants or are concerned about an existing one, the best approach is open communication. By addressing risk factors like smoking, hygiene, and bite pressure early on, we can virtually eliminate the chances of failure. I am committed to helping you achieve a smile that is not only beautiful but also healthy and resilient for years to come.
- Periodontal Disease Stages: From Gingivitis to Advanced - March 30, 2026
- 5 Reasons Your Dental Implant Failed & How to Prevent It - March 23, 2026
- Bone Grafting for Dental Implants: Complete Guide - March 16, 2026
 (310) 859-9449
(310) 859-9449 5 Reasons Your Dental Implant Failed & How to Prevent It
5 Reasons Your Dental Implant Failed & How to Prevent It