As a periodontist, I have dedicated my career to helping patients save their teeth and improve their overall health. When patients sit in my chair, they often feel nervous or uncertain about what is happening inside their mouths. They know something feels “off,” but they aren’t sure of the severity. My goal is always to bring clarity to that confusion. By understanding the health of your gums, you empower yourself to make better decisions for your future.
One of the most important things I explain to my patients is that gum disease is not a static condition. It is a progressive journey. It doesn’t happen overnight, and in many cases, it doesn’t cause pain until it is quite advanced. That is why understanding the stages of periodontal disease is vital. If we catch it early, we can often reverse it completely. Even in later stages, we have incredible technologies and treatments to manage the disease and restore function.
I want to walk you through exactly what happens during these stages, what I look for during an examination, and—most importantly—how we can get your smile back on track.
What Exactly Is Periodontal Disease?
Before we dive into the specific stages, let’s define what we are dealing with. Periodontal disease, commonly known as gum disease, is an infection of the tissues that hold your teeth in place. It is typically caused by poor brushing and flossing habits that allow plaque—a sticky film of bacteria—to build up on the teeth and harden.
When this plaque is not removed, it turns into tartar (calculus), which acts like a splinter in your finger. Your body’s immune system tries to fight off the bacteria living on that tartar. This battle between the bacteria and your immune system results in inflammation. If left untreated, this inflammation destroys the gums and the bone supporting your teeth.
According to the Centers for Disease Control and Prevention (CDC), 47.2% of adults aged 30 years and older have some form of periodontal disease. This data point is startling because it means nearly half of the adult population is walking around with an active infection in their mouth, often without knowing it. The good news is that we can treat it.
The Progression: The Four Stages of Periodontal Disease
When I evaluate a patient, I am looking to categorize their condition into one of four distinct stages. This helps me tailor a treatment plan that is specific to their needs. Here is how the disease progresses from mild to severe.
Stage 1: Gingivitis
The first stage is one you have likely heard of: Gingivitis. This is the only stage of periodontal disease that is completely reversible. At this point, the infection has not yet attacked the bone. It is strictly affecting the soft tissue (the gums).
When I see a patient with gingivitis, they often tell me their gums bleed when they floss or brush. They might notice some redness or swelling, but they rarely feel pain. This lack of pain is tricky because it allows people to ignore the problem. However, bleeding gums are your body’s way of waving a red flag. It is a cry for help.
Signs I look for:
- Red or puffy gums.
- Bleeding during brushing or flossing.
- Bad breath that comes and goes.
- No bone loss on X-rays.
The treatment here is straightforward. We perform a professional cleaning to remove the plaque and tartar you missed at home. Then, we work together to upgrade your home care routine. If we catch it here, your gums can return to a completely healthy, pink, and firm state.
Stage 2: Slight Periodontal Disease
If gingivitis is left untreated, it advances to the second stage: Slight Periodontal Disease. This is the moment the condition changes from “reversible” to “manageable.” The infection has spread beneath the gum line and has begun to destroy the bone.
In my practice, I measure the space between your teeth and gums using a small ruler called a probe. In a healthy mouth, these spaces (or pockets) are 1 to 3 millimeters deep. In Stage 2, I typically find pockets that are 4 to 5 millimeters deep. The bacteria have evolved and become more aggressive, and your body is starting to lose the battle to keep the bone intact.
What is happening biologically?
The bacteria release toxins that irritate the gums. In response, your body produces enzymes to fight the infection, but these enzymes also break down the bone and tissue holding the teeth. It is a double-edged sword.
At this stage, simple brushing and standard cleaning are no longer enough. We usually need to perform a procedure called Scaling and Root Planing (SRP), often referred to as a “deep cleaning,” to remove the bacteria from deep within those pockets.
Stage 3: Moderate Periodontal Disease
As we move to the third stage, the damage becomes more significant. Moderate Periodontal Disease involves more extensive bone loss. The pockets around the teeth deepen, typically measuring 6 to 7 millimeters.
When I examine patients at this stage, the bacteria have not only attacked the bone but also the bloodstream. The bacteria can enter your systemic circulation, potentially affecting your heart and other organs. This is where the systemic link becomes very real.
Symptoms patients notice:
- Gum recession (teeth look longer).
- Sensitivity to hot and cold.
- Consistent bad breath or a bad taste in the mouth.
- Possible slight movement of teeth.
Treating moderate disease often requires more than just deep cleaning. We may need to use advanced techniques, such as laser therapy, to kill the bacteria and stimulate healing. My goal at this stage is to halt the progression immediately to prevent tooth loss.
Stage 4: Advanced Periodontal Disease
The final stage is Advanced Periodontal Disease. This is the most severe form of the condition. At this point, the bone loss is extensive, and the pockets are very deep (over 7 millimeters). The teeth may feel loose, shift out of alignment, or hurt when chewing.
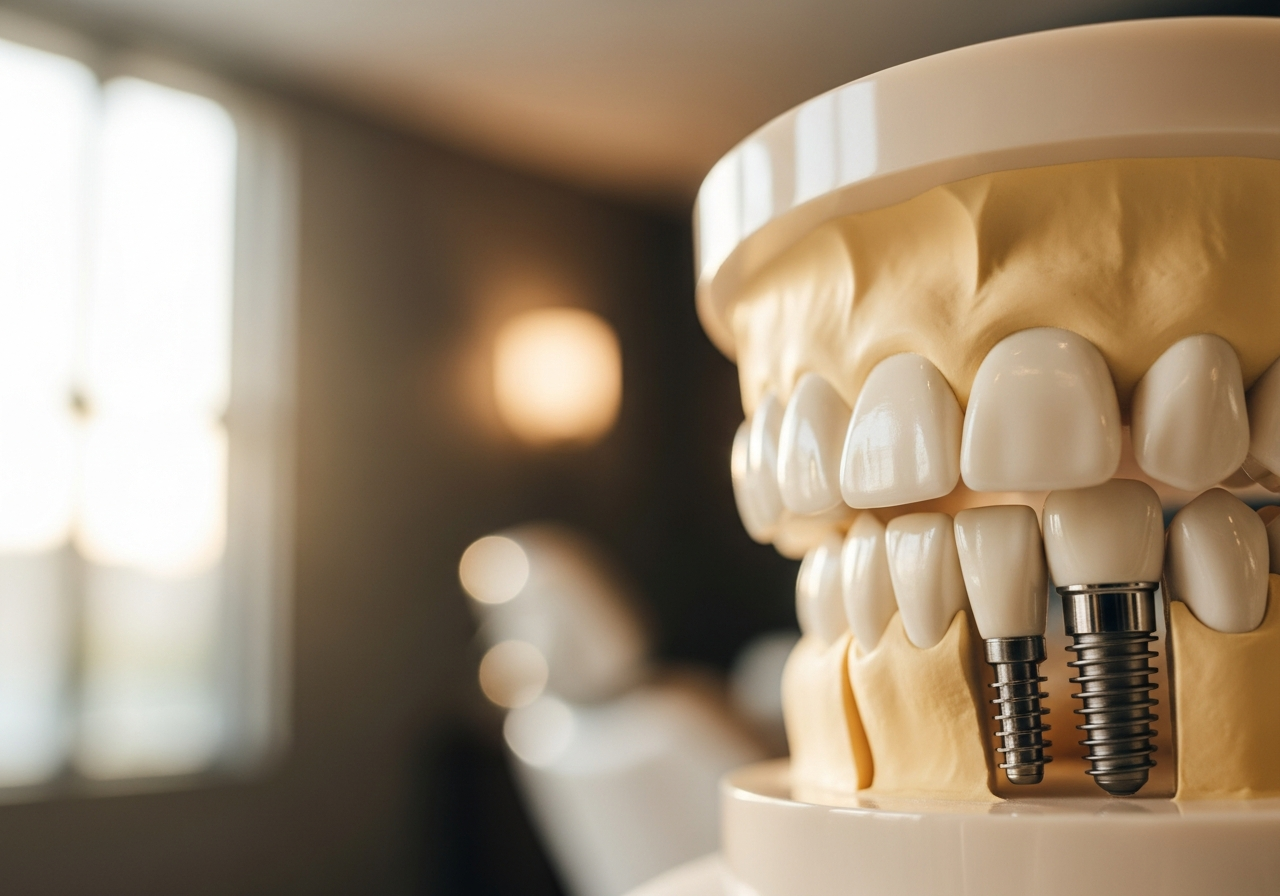
I know this sounds frightening, but I want to reassure you that even at this stage, there is hope. While we cannot grow back the bone that was lost without surgical intervention, we can stabilize the condition. We might need to discuss therapies to regenerate bone or, in some cases, replace hopeless teeth with dental implants to restore full function and aesthetics.
This stage requires a comprehensive approach. It isn’t just about cleaning teeth; it is about rehabilitating your entire oral health foundation.
The Hidden Risks: Who Gets Periodontal Disease?
You might be wondering, “Why did this happen to me?” While plaque is the primary cause, other factors can accelerate the stages of periodontal disease. Understanding your risk factors helps us manage your condition better.
Smoking is the most significant risk factor. Smokers are twice as likely to have gum disease compared to nonsmokers, according to the CDC. Smoking weakens your immune system, making it harder for your body to fight off a gum infection. Furthermore, smoking restricts blood flow to the gums, which can mask the early signs of bleeding, making the disease harder to detect until it is advanced.
Other risk factors include:
- Genetics: Some people are simply more genetically predisposed to gum disease. If your parents lost their teeth early, you might be at higher risk.
- Diabetes: There is a two-way street between diabetes and gum disease. High blood sugar fuels the bacteria in your mouth, and severe gum disease can make it harder to control blood sugar.
- Stress: Chronic stress weakens your immune system, making it harder to fight off infection.
- Medications: Certain drugs can cause dry mouth or gum overgrowth, which increases the risk of disease.
The Body-Mouth Connection
I always tell my patients that the mouth is the gateway to the body. You cannot have a healthy body with an unhealthy mouth. The inflammation associated with the various stages of periodontal disease has been linked to several systemic conditions.
When your gums are inflamed, inflammatory markers enter your bloodstream. Research has shown associations between periodontal disease and cardiovascular disease, stroke, and even adverse pregnancy outcomes. By treating your gums, I am not just saving your smile; I am helping to protect your overall well-being.
For more in-depth information on how oral health impacts your entire body, I recommend reading this article from the Centers for Disease Control and Prevention (CDC). It provides excellent resources on the connection between your mouth and your general health.
How We Treat the Disease: A Positive Outlook
Now that we have covered the scary parts, let’s talk about the solutions. As a periodontist, I have a wide array of tools to treat gum disease, regardless of the stage.
Non-Surgical Treatments
For the earlier stages, we focus on non-surgical methods. Scaling and Root Planing is the gold standard. We numb the area to ensure you are comfortable, and then we meticulously clean the root surfaces of the teeth. This removes the bacterial toxins and creates a smooth surface for the gums to reattach.
We also use antibiotics, either in pill form or placed directly into the gum pockets, to help eliminate lingering bacteria.
Surgical and Laser Treatments
For moderate to advanced stages, we may need to access the bone to clean it thoroughly. However, modern periodontics has come a long way. We now use minimally invasive techniques.
Laser gum therapy is a fantastic advancement. It allows me to vaporize the diseased tissue and kill bacteria without the need for scalpels or sutures in many cases. This results in faster healing and less discomfort for you.
If you have lost bone or gum tissue, we can perform regeneration procedures. Using bone grafts and tissue-stimulating proteins, we can encourage your body to regenerate some of the lost support. It is truly amazing what modern dentistry can achieve.
Prevention: Your Daily Defense
While I am here to treat the disease, my ultimate goal is for you to need me less! Preventing the progression through the stages of periodontal disease starts at home. Here is the routine I recommend to all my patients:
- Brush twice a day: Use a soft-bristled toothbrush and fluoride toothpaste. Angle the brush toward the gum line at a 45-degree angle.
- Floss daily: Flossing is non-negotiable. It cleans the 40% of your tooth surface that your toothbrush cannot reach.
- Use an antimicrobial mouthwash: This adds an extra layer of protection by reducing the bacterial count in your mouth.
- Regular visits: Do not skip your dental check-ups. We can spot the early signs of Stage 1 Gingivitis long before you notice anything is wrong.
Your Journey to Health
I know that reading about bone loss and infection can be overwhelming. However, I want you to leave this article feeling empowered, not fearful. Knowledge is the antidote to anxiety. By understanding the stages of periodontal disease, you are already taking the first step toward better health.
Whether you are noticing a little bleeding when you floss or you are worried about loose teeth, the most important thing you can do is seek professional care. We are not here to judge your past habits; we are here to build your future health. My team and I have helped countless patients restore their smiles and their confidence, and we can do the same for you.
Your gums are the foundation of your smile. Let’s make sure that foundation is strong, healthy, and built to last a lifetime.
- Periodontal Disease Stages: From Gingivitis to Advanced - March 30, 2026
- 5 Reasons Your Dental Implant Failed & How to Prevent It - March 23, 2026
- Bone Grafting for Dental Implants: Complete Guide - March 16, 2026
 (310) 859-9449
(310) 859-9449 Periodontal Disease Stages: From Gingivitis to Advanced
Periodontal Disease Stages: From Gingivitis to Advanced